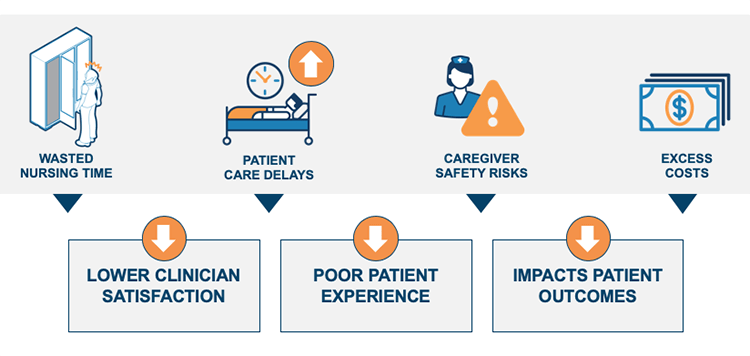
As a healthcare facility, your goals are clear: Provide premium care and keep your patients safe and healthy. This often means accounting for specialized needs among high-risk patient populations. One critical consideration is maintaining skin integrity for less-mobile patients in order to avoid pressure injuries and other adverse events. Every minute a high-risk patient waits on a standard bed increases the risk of skin breakdown. And while specialty surfaces and equipment reliably work to maintain a patient’s skin integrity, unpredictable demand for this specialty equipment too often leads to equipment delays.
Time to therapy: A key metric when it comes to outcomes
The time between when a high-risk patient is admitted to a hospital and when they are placed on a therapy bed and surface is critical to reducing adverse events, such as falls and pressure injuries. For example, recent clinical research demonstrates the average hospital bed places 100mmhg of pressure onto a patient’s tissues. After only two-and-a-half hours, tissues can no longer tolerate the pressure and breakdown can occur.
For most patients who are mobile and move in the bed, this is not a concern. But for the 400-pound bariatric patient or the 90-year-old stroke patient, this timing is critical. Alarmingly, in a survey of wound care clinicians, it was reported the average time between a patient’s admission and being placed on a therapy surface is 7 hours, far beyond the two-and-a-half hours at-risk patients can tolerate.
Avoiding hospital-acquired pressure injuries
Frequently, delays in time to therapy result in entirely preventable hospital-acquired pressure injuries (HAPIs). Hospitals and care facilities do not receive additional reimbursement for the treatment of these injuries, typically absorbing more than $100,000 in unreimbursed costs for each occurrence. Beyond that immediate monetary cost, hospitals must publicly report HAPIs as adverse events — indicators of substandard patient care that deliver ongoing reputation damage. To top this off, pressure injuries are the second leading cause of hospital litigation.
Equipment availability issues impede time to therapy
While most hospitals and care facilities follow best practices for preventing hospital-acquired pressure injuries among high-risk populations, it can be difficult for a facility to accurately predict the volume of high-risk patients they will receive. Variable demand means that purchasing a full complement of specialty equipment is not a cost-effective solution for most hospitals. Rental is a more viable option to meet the immediate demands presented by their high-risk patients or to supplement their existing fleet of available specialty beds and surfaces.
However, the decision to rent puts the responsibility for essential medical equipment entirely in the hands of a third-party partner. Unfortunately, not all rental vendors meet the tight delivery timelines and equipment availability demands required to minimize time to therapy.
Moreover, most hospitals and care facilities lack a centralized equipment management process needed to optimize the use of their owned specialty equipment. This leaves them without the visibility needed to reduce turnaround times and ensure specialty equipment is available and patient-ready, when and where it’s needed.
4 questions to drive equipment availability and reduce time to therapy
If you’re considering renting specialty equipment, remember to vet your rental provider to ensure you’re getting high-quality, patient ready equipment. In the process, there are a few things to consider.:
- Do they have the flexibility to provide the specialty equipment you need, when it is truly needed?
Not only do the types of patients you see each day vary, but the volume differs as well. Ensure your rental provider has ready access to the array of equipment you’re looking for. Also make sure they have the capability to quickly meet the ebb and flow of your census. Confirming both of these can provide peace of mind that your rental provider is supplying equipment only when it is actually needed so you are not overspending on rental. - How fast can the equipment be delivered?
The goal is to shorten the time between admission of a high-risk patient and placement on a specialty surface. The third-party vendor you choose should be located nearby and able to provide rentals quickly to reduce the risk of developing a pressure injury. An often-overlooked element of time to therapy is the ordering process. Your third-party vendor should also help develop ordering algorithms that help your caregivers quickly determine the right specialty equipment needed for different at-risk patient types. - What quality standards are followed?
As with any piece of rental medical equipment, you want to make sure it is clean, patient-ready and maintained to the highest quality standards to help keep your patients safe. And remember, just because a vendor says they’re ISO certified doesn’t mean they’re following the stringent medical equipment guidelines OEMs are required to follow. If you want to brush up on the difference between ISO 13485:2016 and ISO 9001:2015, here’s an infographic you might enjoy. - Are additional services available to increase equipment availability?
Renting equipment might not be the only answer for your facility to ensure patients are placed on the needed equipment in a timely manner. If you have the resources, you should consider how to maximize access to your own specialty equipment through an established, centralized management process. Before you worry about it being an overwhelming burden to develop such a program internally, ask your third-party vendor if bed management is in their wheelhouse. When medical equipment management is done right, hospitals can achieve some powerfully positive outcomes.
If you’re still in the evaluation process, here are some more questions you should ask third-party rental providers during your assessments.
You can also visit our Resource Center to learn more.