After a year of ongoing COVID surges, burnout among healthcare workers is at an all-time high — and this problem is increasingly affecting staff beyond the emergency department (ED) and intensive care unit (ICU). A survey from Mental Health America found that 93% of healthcare workers across hospitals are experiencing stress, while more than three in four report feelings of burnout. Another survey from Berxi found an unnerving 84% of healthcare workers feeling at least somewhat burned out — and nearly half considering quitting.
Pouring Gasoline on Nurse Burnout
Even before the pandemic, estimates suggested as many as four in 10 nurses were already reporting feelings of burnout. The nation heralded nurses as heroes on the frontlines as they faced the first wave of the pandemic. But even as vaccination shows progress in minimizing COVID cases, nurses continue to see elevated patient surges that threaten to leave them short-staffed, all while managing the emotional weight of seeing the toll of the pandemic up-close. A growing body of academic research is validating pandemic-amplified nurse burnout.
But it’s not just ED and ICU nurses. A recently released Advisory Board report showed burnout levels increased by more than 200% compared to where it was pre-pandemic across all nursing staff. In fact, nursing teams throughout hospitals and health systems are increasingly short-staffed and feeling under-supported as they deal with rapidly fluctuating patient volumes, higher demands around infection control and navigating their own exposure risks.
HTM Burnout: An Overlooked Component of Pandemic Fallout
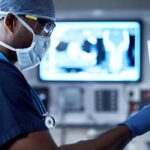
It’s not only nurses and other clinical staff who are feeling stressed, overwhelmed and experiencing burnout as a result of the pandemic. Other teams within the hospital are facing the same imbalance of heightened demands pressing against resource and staffing constraints. One key example is clinical engineering and biomedical teams — those responsible for ensuring the availability and performance of essential medical devices and equipment, like the ventilators that dominated headlines a year ago.
In response to those shortages and patient volume surges, most hospitals acquired additional equipment to meet peak-demand pressures. As they purchased or rented equipment to increase their onsite inventories, they exposed another, deeper problem: biomedical teams in many hospitals were already short on resources needed to maintain, repair and manage logistics for rapidly growing inventories of medical equipment. Like nurses, Healthcare Technology Management (HTM) staff had already been experiencing higher levels of burnout before the pandemic — compounded by a long-standing talent shortage. Today, biomed teams are managing larger equipment inventories, more unpredictable demands and higher budget pressures — adding stress that’s worsening the HTM burnout problem.
Supply Chain Teams Under New Pressures
The pandemic made us all acutely aware of the tricky, no-margin-for-error high-wire act that is the global supply chain. We experienced a toilet paper crisis at home and a PPE crisis in hospitals. This cast hospital supply chain teams into the spotlight as never before, as they worked to move mountains to locate and expedite arrival of critical equipment and supplies during the unprecedented stress of the early months of the pandemic.
Today, most hospital supply chain teams have gained a better handle on how to manage ongoing demand surges and sporadic supplier shortages. Moreover, healthcare organizations — like their peers in other segments — are more readily shifting away from the traditional “just in time” model and toward a “just in case” model. But even as hospitals accept the need to spend more to maintain larger inventories, supply chain teams remain under intense pressure to reign in additional costs. They’re also feeling the emotional stress of remaining in the spotlight — feeling more immediately responsible for mitigating clinician and Healthcare Technology Management stress by making sure they have the equipment they need, and more acutely aware of how successful supply chain strategies directly impact patient outcomes.
A Problem Vaccines Can’t Solve
The common theme with these examples of increasing staff burnout is that the pandemic isn’t the sole cause of the problem. Rather, the pandemic amplified existing pressures and exposed operational flaws that leave healthcare workers across the hospital feeling under-supported and overwhelmed.
Yet, the pandemic also offers a potential inflection point: As hospitals and health systems recover, rebuild and restructure, there is a tremendous opportunity to fundamentally re-think how smarter operational strategies can better support their staff.
Read how some hospital networks are addressing staff productivity and satisfaction by unraveling equipment availability issues and building smarter strategies for managing essential medical equipment.