The increasing adoption and use of medical lasers has, unsurprisingly, brought increasing attention to developing best practices and safety standards from regulatory agencies. But is your operating room up to code? Part 3 of a 4-part series exploring the gaps surrounding medical equipment quality.
Rising Regulatory Standards for Laser Safety
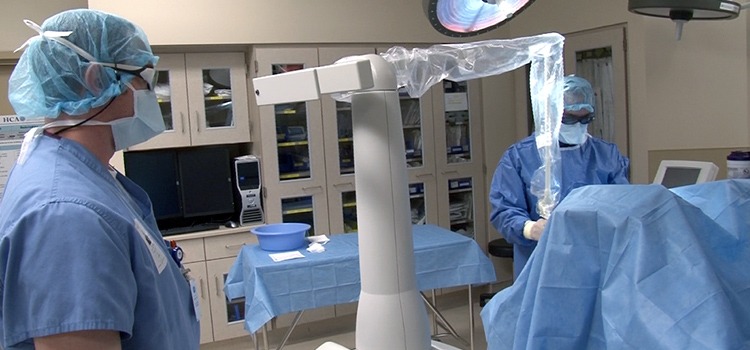
Growing demand for more precise, less-invasive treatments is turning medical lasers into mainstream tools in the modern OR — a promising technology with rapidly expanding applications. However, as healthcare facilities expand their use of medical lasers, new ANSI safety standards and AORN guidelines will require many organizations to make major changes in their laser operation protocol. These new requirements present significant staffing challenges, as well as ongoing training and administrative burdens — which few operating rooms fully understand or are prepared to handle.
The increasing adoption and use of medical lasers have unsurprisingly brought a corresponding increase in attention to developing best practices and safety standards. OSHA, The Joint Commission and AORN now all play a role in adopting and enforcing safety standards created by the American National Standards Institute (ANSI), the leading independent organization that develops standards and recommended practices for the safe use of many medical technologies, including medical lasers.
Approximately 70% of hospital laser programs assessed by Agiliti do not meet new ANSI laser operator certification standards.
ANSI has continually updated its standards for the safe use of medical lasers over the past 30 years, but the last few years have seen changes that every healthcare organization should know about. These changes can be broken into three distinct elements:
- Laser Safety Program and Laser Safety Officer (LSO) requirements
- Dedicated & Fully Trained Laser Operators
- Third-Party Laser Use
1) Laser Safety Program and Laser Safety Officer (LSO) Requirements
To be compliant with the American National Standards Institute (ANSI) Z136.3 Standard for “Safe Use of Lasers in Health Care,” every facility that uses a medical or aesthetic laser must establish a formal Laser Safety Program that is documented and managed by an appointed Laser Safety Officer (LSO). Here are the key points you need to know:
LSO Requirements
ANSI Z136.3: Laser Safety Officer 1.3 and Administration 5.1
What it Says:
Every facility that uses a medical or aesthetic laser must establish a formal Laser Safety Program that is documented and managed by an appointed designated Laser Safety Officer (LSO). The standard applies to all patient care cases in which a laser is used, regardless of whether the laser system is owned, borrowed, or rented.
What You Need to Know:
-
- Each facility must establish and maintain a Laser Safety Program and designate an in-house LSO, and if deemed necessary, additional personnel such as a Deputy LSO (DLSO)
- A third-party provider of laser and operator services does not serve as a facility’s LSO by virtue of being the provider of laser rental services. Oversight and operation are two separate tasks
- The LSO is responsible for ensuring that appropriate laser safety education and training is provided and documented
Medical Laser Safety Officer (MLSO) Requirements
ANSI Z136.3: Personnel 5.2.1
What it Says:
The LSO has the training and experience to administer a laser safety program. LSO education and preparation should include, but not be limited to, completion of a formal medical laser safety course, completion of a formal MLSO course, and certification as a MLSO (recommended).
What You Need to Know:
-
- In-house LSO should now also be trained and certified as a Medical Laser Safety Officer
- Certification is attained from the Board of Laser Safety (BLS)
- Approved training courses are offered through the Laser Institute of America
- In-house LSO should now also be trained and certified as a Medical Laser Safety Officer
2) Dedicated and Fully Trained Laser Operators
Because medical lasers are still an emerging specialty technology, most healthcare facilities have taken an organic or ad hoc approach to meeting OR staffing needs for operating medical lasers. However, recent standard recommendations place new requirements on laser operators:
Dedicated Laser Operators
ANSI Z136.3: Administrative and Procedural Controls 4.2.5
What it Says:
Procedural Controls include “Assigning a dedicated person to operate the controls, if applicable, when appropriate for the procedure and practice setting. The laser operator should not have competing responsibilities that would require leaving the laser unattended during potential operation.”
What You Need to Know:
-
- Many facilities assign laser operator duties to the circulating nurse that also has other patient-care responsibilities.
- This common approach is non-compliant with the latest standards. The split responsibilities of the circulator being the laser operator can pull attention away from safe use standards designed to protect both staff and the patient.
Fully Certified and Trained Laser Operators
ANSI Z136.3: Training Programs 5.2.2
What it Says:
Laser safety training programs shall provide a thorough understanding of all procedures required for establishing and maintaining a safe environment during the use of a health care laser system (HCLS). Training shall be specific to the HCLS in use and the procedures to be performed.
What You Need to Know:
-
- Laser operators need to hold certification of training on both the laser system and the procedure being applied.
- Many facilities do provide training on the technology, but not the specific procedures. For example, training on a Holmium laser does not differentiate between using the technology for a Bronchoscopy and a Ureteroscopy. As a result, approximately 70% of hospital laser programs assessed by Agiliti do not meet the updated standards.
3) Third-Party Laser Use
To manage dynamic case volume and rapidly evolving laser technologies, healthcare organizations increasingly leverage third-party medical laser services. Best-in-class partners do everything from delivering and servicing the medical laser platforms to providing certified technicians to operate the devices. However, revised ANSI standards make it clear that the onus for third-party quality assurance lies with the facility’s LSO.
Third-Party Laser Services
ANSI Z136.3: Third Party Laser Use 1.4.2
What it Says:
If the user employs a third party to provide a health care laser system (HCLS) (often including the operator and all accessory equipment), the laser safety officer or designee shall assess the rented or borrowed equipment for compliance with all federal, state and local requirements, as well as compliance with all requirements listed in ANSI Z136.3.
The laser safety officer shall ensure that the terms of agreement between the third-party provider and the health care facility include, but are not limited to:
-
- The credentials of the third-party laser operator meet the facility’s policy.
- The health care facility has received written validation of the maintenance, service, cleaning and condition of the equipment.
- Data and elements of documentation collected by the third party are appropriate, meet the health care facility policy, and can be verified by facility health care provider.
- All health care providers expected to be in the room with the third-party laser provider have had adequate training on all equipment, in order to safely operate the equipment in the absence of the third-party employee, thereby ensuring safe patient care at all times.
What You Need to Know:
-
- Third-party providers need to retain and provide useful key performance indicators to assist the facility’s LSO in program oversight and continuous improvement initiatives and to comply with accreditation standards. But not all third-party providers present or allow access to maintenance records for the lasers they bring into the facility or have sufficient quality indicator data of their service provision on a quarterly basis.
- The laser safety officer or designee need to approve each laser and laser operator that comes into the facility. That does not mean they need to approve each laser or operator each time they come in, but they should sign off on the operator’s credentials, laser condition and maintenance records prior to its use at the facility.
- Third-party providers should provide an annual in-service for any facility staff that work in or around the laser so the facility can meet ANSI requirements.
Why it Matters: The Impacts of Non-Compliance on the Quality Engine
As agencies like OSHA and The Joint Commission begin enforcing the elevated ANSI laser safety standards, non-compliance will become a real risk, both financially and from a brand reputation standpoint. But the lack of a fully compliant Laser Safety Program in most hospitals presents a much more immediate set of risks.
Patient and staff safety incidents
As medical technologies grow increasingly powerful, improper and/or unsafe use can lead to serious safety incidents that impact both patients and OR staff. Along with opening up the facility for lawsuits and litigation.
Malfunctions and case delays
Even if a hospital dodges a safety incident, equipment malfunctions resulting from improper use or inability to successfully troubleshoot system errors can lead to costly and sometimes unnecessary repairs — and much more costly case delays.
The quality engine
The Quality Engine we introduced in the first blog post of this series is incredibly relevant here. The OR is a major revenue center in most healthcare organizations — not to mention a high-visibility area from a brand reputation standpoint. Beyond the immediate costs of case delays or safety incidents, these events have cascading impacts on the OR Quality Engine — damaging patient and staff satisfaction, reducing reimbursements and operational efficiency, etc. — that impact profitability and growth in complex and long-lasting ways.
The Challenges of Trying to Maintain Compliance In-House
The risks and costs of non-compliance should lead all hospitals to take the new ANSI standards seriously. But unfortunately, achieving compliance comes with its own set of challenges and costs:
- Aligning Laser Operator Staffing with Fluctuating Case Demand: Case demand can vary significantly on any given day. For example, on one day, an 11-hospital system (an Agiliti customer organization) required seven (7) dedicated laser operators across 22 hours of the day to cover its medical laser case demand. The next day, that number was zero. Many hospitals will find it difficult to adequately predict the staffing needed to cover both the maximum case demand and low-demand days.
- Exponential Training Demands: The technology- and procedure-specific training requirements of the new ANSI standards rapidly multiply the staffing burden. That same 11-hospital system performs six different procedures, and while several hospitals use the same type of laser, each of the 11 hospitals has a unique model. To ensure their dedicated laser operators can cover peak case demand at any of its hospitals, each laser operator must be properly trained and certified on 60+ devices and procedures — including rarely performed procedures.
- Administration of Laser Operator Scheduling & Training: A hospital will also need to dedicate staff for laser operator scheduling to maximize staffing efficiency and minimize case delays. This can become a very complex process matching the certified laser operator with the correct case. And to achieve full compliance with ANSI standards, hospital administrators are also responsible for creating and maintaining laser safety logs, safety documentation and ensuring ongoing compliance in practice with all laser safety standards.
All of these factors contribute their own substantial headaches and costs. And as mentioned, falling short on any of these can not only put a hospital at risk of non-compliance penalties and embarrassments — it can actually put staff and patient safety at risk.
Read the Full Report Today
Want to learn more? You can download the full report today — from the nuances in ISO standards and how they impact patient safety, to tips for how to choose vendors that best support the delivery of quality clinical outcomes and exceptional patient experiences.
Visit our Resource Center to discover more, or return to the blog menu.